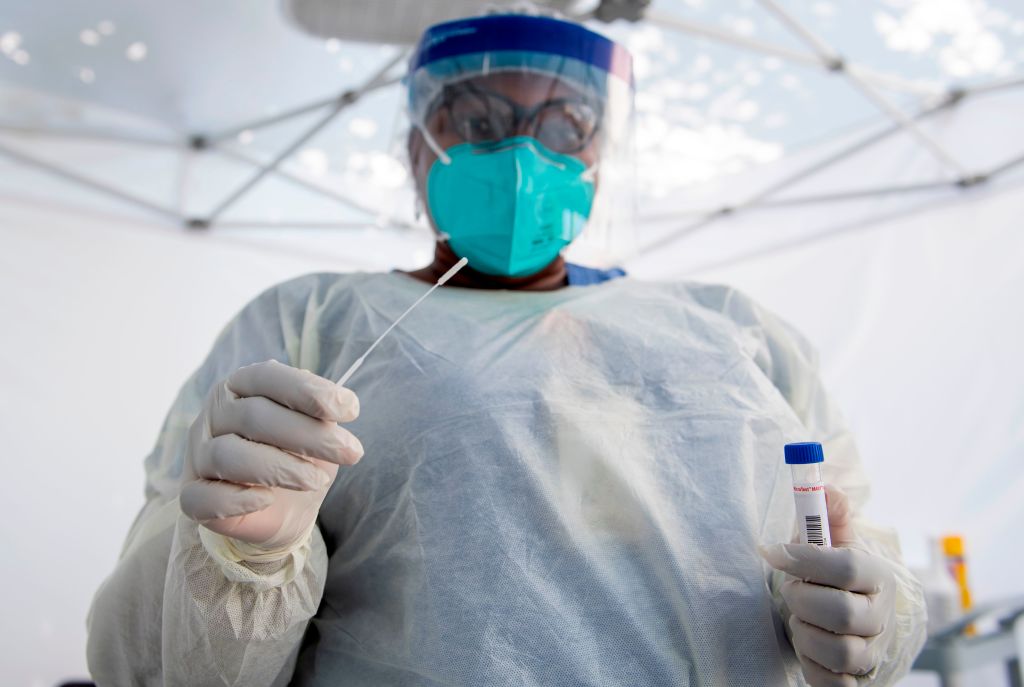
A student in Florida waited 11 days. Positive. A 14-year-old in California waiting for 24 days. Negative. A New York writer has been waiting for four days and still waiting. As the United States struggles to control the use COVID-19-pandemic Twitter people across the country to announce the arrival of their virus test results. The point of these tweets is not only to convey the same result, but the absurdity of receiving so stale a result that is almost completely useless from the point of view of public health. Social Media messages of July and August are a clear frustrating reality: some Americans get their results in a couple of hours, while other days to wait weeks. To illustrate the problem, make a card out to create shows average time of times the waiting test results across the country. What we found was rather that waiting times not only a geography product, but also from a chaotic, a disparate system of laboratories and agencies around struggling with supply difficulties, logistical challenges and a lack of federal leadership. Chaos is virtually impossible to cleanly map and track, but what we have on the road, reveals a fundamentally broken system learned that the country’s ability to respond effectively to the pandemic is hindered. If a person COVID-19 is tested in the United States, it is not always clear where the sample of saliva or nasal swab will end. About half are sent to hospital laboratories, university laboratories and public laboratories occupied by more than 700,000 samples per day. The other half is sent to 12 major commercial laboratories, including Quest Diagnostics, LabCorp and Aegis Sciences Corp., which many institutions across the country, some states or regions served. At the beginning of the pandemic Testing conducted by the hospitals to the US Centers for Disease Control and Prevention and other public laboratories that sent serve as a first line of defense when an outbreak is. But public laboratories run small operations and not able to handle the kind of mass tests required in this pandemic. Since the federal government pushed through community-based drive for further testing and test sites launched, commercial laboratories were to jump in an optimal position. They already had relationships with pharmacies and other retailers that manage existing sites as well as hospitals, clinics and clinics that do not have their own laboratories. Over 30 million COVID-19 samples were passed through commercial laboratories, since the federal government on February that the work to do in 29. But the system as a whole has been started is not ready for such an acceleration ramp without previous. Addressing the lack of nasal swabs, reagents, qualified personnel, and test the machines was a game of Whack-a-Mole. If the supplies can not be delivered, a laboratory, which has already received so many tests as they can handle inevitably fall behind. Laboratories across the country and manufacturers can fairly quickly one can not act quickly enough to deliveries. “It ‘Hunger Games for laboratories,” says Rachael Liesman, Director of Clinical Microbiology at the University of Kansas Hospital. “If we get our supplies, then we can operate, and if we do not succeed, it will stop.” Read more: drop crown test numbers, the reality of US pandemic actually veiled addition, US labs are not set, work together to ease, making it difficult to predict where the next pop-up bottleneck. Nada Sanders, professor of supply chain management at Northeastern University, said that without a competent national authority to monitor all the moving parts, every step of the US control system, including the testing laboratories and manufacturers, will continue to be overwhelmed. “And ‘extremely uncoordinated,” says Sanders. “We have completely open markets. When it comes to public health, which is not something that is based on free market forces”. The Federal Emergency Management Agency (FEMA) is working with the states in an effort to allocate resources as needed. But because national reserves Dry Run, FEMA supplies is to buy from the same suppliers as the laboratories to provide additional resources for the competition. FEMA sends supplies to the states of reception, which then send them to laboratories. But health policy experts and laboratory directors said in an interview with time, it is unclear how many supplies procured FEMA and how to distribute them States. The random national system delays currently operates rings. In mid-July, only 37% of the tests across the country came in a day or two back, according to a recent report by researchers at Northeastern, Harvard, Rutgers and Northwest University. As with the other tests it took four to seven days 21% 29% 3 days lasted and the remaining 13% have more than a week. The data of the Department of Health and Human Services also show delays. In July, only 45% of laboratory tests were in three days or less complete. orbital period it started completed within three days to improve the last week of July with 56% of the test. But the lab times vary, which is why people in the region are explained to experience different waiting times: a person who is being tested at a facility works doctor with a hospital laboratory, is simply another tail like a person involved in a chain of pharmacies work goes to a commercial laboratory. The lack of test equipment has left scrambling laboratory directors. “The supply chain for diagnostic manufacturers can not keep up with demand,” said David Dexter, CEO and President of Sonora Quest Laboratories, a joint venture between Banner Health and Quest Diagnostics. The five company sites in Arizona together hold 70% of COVID-19 tests in the state. “We failed to show seven to 10 days. For us this is not acceptable.” What happened Sonora Quest shows the fragility of the system. Last April, when stay-at-home orders were still in place and testing have been reserved for in-patients and health care providers, the demand was relatively low; the company is only about 1,000 tests per day this month. try to expand Dexter lobbying the health department of the state, more patients like them to know in his laboratory of long-term care facilities, the burden can bear. Then, on May 15, in Arizona he ended his stay-at-home order. The number of cases increased from about 40,000 to 100,000 over the 4th of July weekend. In the same period, the positivity rate of 6% jumped to 23%. At its peak in early July Sonora Quest was receiving 14,000 samples per day if its capacity was 10,600. The company has more needed supplies, but Sonora three vendors were already stretched thin. To make matters worse, Sonora supply of reagents has been a day could be a consequence of FEMA to 6,000 tests reduced supply of reagents to hotspots around the nation assigned country. Sonora tried Offload Test for Quest laboratories in other states, but they were already full. Workshops on the east coast, not with Quest connected, offered to take about 1,000 tests, but Dexter says that a tooth had not done in Sonora residue, especially since it would take some time, the back-end lab tech at achieving compatibility between systems. The Sonora challenges they face in this troubling time yet the company. On August 5, the state of Sonora has sent a cease and desist letter for not having exact times for consumers and health care providers to disclose. However, the letter shows that “seems to improve the situation.” Sonora said he has provided about his delivery provide accurate information, but went on to comment on the letter. Sonora Quest is not unique. In addition to the competition tests and laboratory delivery across the country also competing for market share and money. In May, the New York Times reported on a series of smaller workshops that were under the operating capacity, while large laboratories have their limitations. “The big companies are not just saying, we have business more, we will send it over them ‘”, says Sanders, the expert supply chain. Although the workshops were a way to spread the load more evenly, without losing revenue, other obstacles in the way. For example, if a laboratory device used a new word, a different type of buffer or reagent it must demonstrate that the results are reliable. Since the shortage began their laboratories diversified test instruments because their usual suppliers are flooded. The result is that the changes make it difficult to collaborate in supplies much without introducing further regulatory delays. (It also shows how the experience of Dexter, laboratory systems are designed to communicate with their typical clients such as doctors’ offices and pharmacies, not necessarily with each other.) Some laboratories, such as the University of Kansas Hospital, where Liesman work, try working with its existing technology. When his lab tests in hospitals receive the various instruments of the patient-tracking have, the staff at the two hospitals have to enter all the information manually. This allows COVID-19 samples are divided, but also slows everything down in a time when laboratories are against the clock race. “The pandemic has revealed many deficiencies in the system”, says Liesman. “It ‘a nightmare from the laboratory point of view.” Alarmingly, the exam questions have so-US are considerably above that people simply do not take the test, probably out of frustration with delays. In the first week of August, when 50,000 new cases each day nationwide have been reported in the application of US test actually went 9.1%, equivalent to about half a million tests from the previous week. That first drop in demand since the beginning of March scored after COVID project tracking. Some of the decline can be attributed to Hurricane Isaias temporarily close examination some government officials in the Southeast forced. But the material can be held responsible for a defective system only. California, for example, has shown that the results of the report on the state of IT systems hindered unreliable. And several states, in an attempt to clear the backlog, have established that they get tested restrictions. The rules often preclude asymptomatic persons are to reduce the total number of tests, but as much as 40% of COVID-19 cases are asymptomatic, failed to test people who seem to have a large number of cases, the healthy risks missing. In Arizona, says Dexter Sonora Labs for more samples is ready, but they are simply not in the same amount that presents company receives 60% fewer tests from its peak a month ago. “This is a function of the fact that people for 13 hours at very high heat waited in line and then get any result for 7 to 10 days,” says Dexter. None of this bodes well for a policy of containment “people do not want to go through.”. The widespread testing, including testing of asymptomatic individuals is critical for containment infection rates. But the tests are only useful if the results are within one or two days to spare after the 16 study in July by researchers at universities in the Netherlands, the United Kingdom and Portugal. The results, which were published in The Lancet, found that control efforts complementary viruses such as contact tracing and containment were much less effective delayed after the results of three days of testing. If the US backlog is a result of a patchwork system, it should not be surprising that many solutions seem administrative tape. Last week, banded together a group of seven states to a new testing strategy to achieve a whole. The bipartisan agreement, led by the governor of Maryland and joined by the governors of Virginia, Louisiana, Massachusetts, Michigan, North Carolina and Ohio, states allowed fast test kits crown together to buy. This test takes about 20 minutes to process, which means that much larger swathes of the population to get instant results. The disadvantage of these tests is that they are less accurate. But experts have argued that only 50% of cases to identify the total population is better than the approximately 10% of the cases probably identified in the current process. For its part, Sonora Quest in Arizona has spent $10 million in new equipment immune euro, a German supplier and sets and 200 employees trained to investments Dexter Sorona hopes will avoid some of the restrictions of the US power system. He says that by the end of this month Sonora is processing 60,000 COVID-19 tests a day, capable of six times. He is also optimistic that he’ll be able Quest Labs regions need to cooperate hotspot do even with arrears of their own. “It ‘been a risk, but I had to do it,” says Dexter. “It was to dig the only way out.” Picture copyright by Valerie Macon AFP / Getty Images
Related Post
COVID-19 is devastating even nursing homes. The administration Trump does not do much to stop it
At least 75,000 Americans in nursing homes and other structures have long-term care as soon as they died COVID-19 and the devastation is far from...
More than half of Americans fear that the pressure of the White House for a coronavirus vaccine will Rushed
For weeks, the US president Donald Trump has repeatedly forecasts, sometimes bordering on promises that a COVID-19 vaccine is imminent. "We remain on track to...
COVID-19 has killed nearly 200,000 Americans. How many more lives will be lost before the US makes it right?
Forty-five days before the announcement of the first suspected case of what the COVID-19 would be known, the global index of the Health Security has...
Nearly 2 million fewer US teens are vaping now than last year, the data show CDC
Nearly 2 million fewer US teens report on e-cigarettes in 2020 compared to 2019, according to new data from the US Centers for Disease Control...
The Great Race Vaccine: The unprecedented rush to immunize the world against COVID-19
The smarter enemies thrive on surprise attacks. Virus and crown in particular are well aware. remain hidden in animal hosts for decades, sometimes mutate constantly,...
Zeneca has taken its COVID-19 vaccine trial after a break for the security check
This story has been updated to reflect AstraZeneca's investigational vaccine shot. AstraZeneca, the British pharmaceutical company behind one of the most promising candidates COVID-19 vaccine...